The eLitMed.hu medical portal uses computer cookies for convenient operation. Detailed information can be found in the Cookie-policy.
Clinical Neuroscience - 2019;72(03-04)
Content
L-arginine pathway metabolites can discriminate paroxysmal from permanent atrial fibrillation in acute ischemic stroke
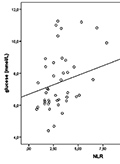
Background - Atrial fibrillation (AF) is the most common arrhythmia diagnosed in clinical practice. We aimed to measure the L-arginine pathway metabolites as well as their ratios in patients with different types of AF or sinus rhythm and to explore the relationship among the markers and clinical variables in the subacute phase of acute ischemic stroke (AIS). Methods - A total of 46 patients with AIS were prospectively enrolled. The patients were divided into three groups based on diagnosis of either sinus rhythm, paroxysmal or permanent AF. Plasma concentration of the L-arginine pathway metabolites were analyzed at post-stroke 24 hours in the three rhythm groups. Besides, clinical variables and laboratory data were recorded. Results - Asymmetric dimetylarginine (ADMA) was significantly higher in patients with permanent AF compared to sinus rhythm (p<0.001). Both ADMA (p<0.001) and symmetric dimethylarginine (SDMA) (p<0.002) at 24 hours were significantly higher among patients with permanent AF compared to those with paroxysmal AF. The L-arginine/SDMA (p<0.031) ratios at 24 hours were significantly higher among patients with sinus rhythm compared to those with permanent AF. ROC analysis also revealed that plasma SDMA cut-off level over 0.639 μmol/L discriminated permanent AF from paroxysmal AF or sinus rhythm with a 90.9% sensitivity and 77.1% specificity. Neutrophil-lymphocyte ratio also showed significantly higher value in individuals with both paroxysmal and permanent AF (p=0.029). Conclusions - Plasma level of SDMA could discriminate permanent from paroxysmal AF in the subacute phase of ischemic stroke. In addition, an increased neutrophil-lymphocyte ratio may suggest inflammatory process in the evolution of atrial fibrillation.
Incidental intracranial lipomas: Assessment of 163 patients
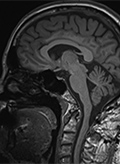
Intracranial lipomas (ILs) are rare congenital lesions which consist 0.1-0.5% of intracranial lesions. They are usually asymptomatic. Our serial of 163 patients is the largest IL serial in literature. Files of the patients who were diagnosed with IL at outpatient clinic of neurosurgery between 2009 and 2018 were screened retrospectively. A total of 163 patients were detected to have been diagnosed with IL according to radiologic findings between 2009 and 2018. Of the patients, 96 were female and 67 were male. Intracranial lipomas are self-limited, slowly growing benign lesions which do not cause a mass effect. We believe that the present study would be a main source due to the currently available insufficient number of studies in literature.
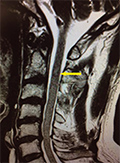
[Prognostic factors of surgically treated spinal meningeomas and long-term surgical outcomes ]
[Introduction, the aim of article - The spinal meningeomas are one of the most common types of spinal tumors. In the treatment of spinal meningeomas, the surgical removal is the gold standard method. There are many factors that have impacts on surgical outcomes such as age, preoperative neurological condition, the extent of resection and histological grade. The aim of our article is to analyze surgical experiences, prognostic features and long-term surgical outcomes of spinal meningeomas. Patients and methods - Retrospective database of surgically treated patients with spinal meningeomas between 2008 and 2016 was made in the National Institute of Clinical Neuroscience, Budapest, Hungary. Demographic data, preoperative neurological symptoms, radiological discrepancies, pathological results (histology, grade), types of treatments and postoperative results were examined. All of our patients were followed clinically and radiologically in the postoperative courses. Results - All of the 153 patients were surgically treated. We have examined 112 women and 41 men. The average age of the patients was 65.5 years. In 98.7% of the cases, the postoperative control examinations (postoperative 6th week) showed a significant improvement in sensorial and motorial functions. The neurological improvements were evident right after the surgeries. In 2 cases (1.30%), no changes were observed in the preoperative symptoms. Recurrence was noticed in 4 cases (2.61%). Conclusion - According to our results, the spinal meningeomas can be sufficiently treated with early diagnosis and total surgical removal. Most of the patients become asymptomatic and the rate of recurrence is quite low.]
EEG-based connectivity in patients with partial seizures with and without generalization
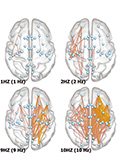
Objective - to investigate the neurophysiological basis of secondary generalization of partial epileptic seizures. Patients and methods - inter-ictal, resting-state EEG functional connectivity (EEGfC) was evaluated and compared: patients with exclusively simple partial seizures (sp group) were compared to patients with simple partial and secondary generalized seizures (spsg group); patients with exclusively complex partial seizures (cp group) were compared to patients with cp and secondary generalized seizures (cpsg group); the collapsed sp+cp group (spcp) was compared to those who had exclusively secondary generalized seizures (sg group). EEGfC was computed from 21-channel waking EEG. 3 minutes of waking EEG background activity was analyzed by the LORETA Source Correlation (LSC) software. Current source density time series were computed for 23 pre-defined cortical regions (ROI) in each hemisphere, for the 1-25 Hz very narrow bands (1 Hz bandwidth). Thereafter Pearson correlation coefficients were calculated between all pairs of ROI time series in the same hemisphere. Z-scored correlation coefficients were compared at the group level (t-tests and correction for multiple comparisons by local false discovery rate, FDR). Results - Statistically significant (corrected p<0.05) EEGfC differences emerged at specific frequencies (spsg > sg; cpsg > cp), and at many frequencies (sg > spcp). The findings indicated increased coupling between motor cortices and several non-motor areas in patients with partial and sg seizures as compared to patients with partial seizures and no sg seizures. Further findings suggested increased coupling between medial parietal-occipital areas (structural core of the cortex) and lateral hemispheric areas. Conclusion - increased inter-ictal EEGfC is associated with habitual occurrence of secondary generalized seizures.
The yield of electroencephalography in syncope
Introduction - Syncope is defined as a brief transient loss of consciousness due to cerebral hypoperfusion. Although the diagnosis of syncope is based on a thorough history and examination, electroencaphalography (EEG) is also an important investigational tool in the differential diagnosis in this group of patients. In this study we aimed to identify the diagnostic value of EEG in patients with syncope. Methods - We retrospectively examined EEG recordings of 288 patients with the diagnosis of syncope referred to the Cankiri State Hospital EEG laboratory, from January 2014 to January 2016. The EEG findings were classified into 6 groups as normal, epileptiform discharges (spike and sharp waves), generalized background slowing, focal slowing, hemispherical asymmetries, and low amplitude EEG tracing. The EEGs were separated according to gender and age. Results - Total of 288 patients were included in this study, 148 were females (51.4%) and 140 (48.6%) were males. Among all the EEG reports, 203 (70.5%) were normal, 8 of them (2.8%) showed generalized background slowing and 7 (2.4%) demonstrated focal slow waves. Epileptiform discharges occured among 13 patients (4.5%). Hemispherical asymmetries were detected in 10 patients (3.5%) and low amplitude EEG tracing in 47 patients (16.3%). There was no significant difference between age groups in EEG findings (p=0.3). Also no significant difference was detected in EEG results by gender (p=0.2). Discussion - Although the diagnosis of syncope, epilepsy and non-epileptic seizures is clinical diagnosis, EEG still remains additional method
[Epidemiology, cost and economic impact of cerebral palsy in Hungary]
[Objective - The purpose of our communication was to determine the total cost of cerebral paretic patients in Hungary between 0 and 18 years and to assess their impact on the national budget. Methods - Based on the data of Borsod county we calculated the CP characteristics. The cost of CP was determined by routine care of individuals. Lost Parental Income and Tax were calculated on the basis of average earnings. The ratio of GDP, Health and Social Budget and Health Budget to CP is based on CP annual average cost and frequency. We have developed a repeatable computational model. Results - Of the risk groups, premature birth (30.97%), low birth weight (29.64%), perinatal asphyxia (19.47%) were the most common. Source is unknown of 37.61% of the cases. CP prevalence was 2.1‰. The two-sided (59.7%) and the one-sided (19.0%) spastic pareses dominated. The most serious form is the two-sided spastic paresis (42.5% GMFCS 3-5 degrees). Epilepsy was 22.0%, incontinence was 27%, mental involvement was 46%. Care for one child up to 18 years of age costs an average of 73 million HUF (€ 251,724). The lost family income was 27.36 million HUF (€ 94,345), and lost tax and health care contributions were 14.46 million HUF (€ 49,862). Additionally, 0.525% of the GDP, 0.88% of the full health and social budget and 1.83% of direct medical costs were spent for CP families. Conclusion - The cost of CP disease is significant. Costs can be reduced by improving primary prevention. From the perspective of the family and government, it is better to care for families so they can take care of their disabled children.]
[Rehabilitation possibilities and results after neurosurgical intervention of brain tumors ]
[Objectives - Authors examined the rehabilitation possibilities, necessities, and results of patients after operation with brain tumor, and report their experiences. Method - Retrospective, descriptive study at the Brain Injury Rehabilitation Unit, in National Institute for Medical Rehabilitation. Patients - Patients were admitted consecutively after rehabilitation consultation, from different hospitals, following surgical intervention of brain tumors, between 01 January 2001 and 31 December 2016. Patients participated in a postacute inpatient rehabilitation program, in multidisciplinary team-work, leaded by Physical and Rehabilitation Medicine specialist included the following activities: rehabilitation nursing, physical, occupational, speech, psychological and neuropsychological therapy. Results - At the rehabilitation unit, in the sixteen-year period 84 patients were treated after operation with brain tumor. Patients arrived at the unit after an average of 41 days to the time of the surgical intervention (range: 10-139 days), and the mean length of rehabilitation stay was 49 days (range: 2-193 days). The mean age of patients was 58 years (20-91), who were 34 men and 50 women. The main symptoms were hemiparesis (64), cognitive problems (26), dysphagia (23), aphasia (16), ataxia (15), tetraparesis (5), and paraparesis (1). The mean Barthel Index at the time of admission was 35 points, whereas this value was 75 points at discharge. After the inpatient rehabilitation, 73 patients improved functionally, the status of 9 patients did not show clinically relevant changes, and 2 patients deteriorated. During the rehabilitation 10 patients required urgent interhospital transfer to brain surgery units, 9 patients continued their oncological treatment, two patients continued rehabilitation treatment at another rehabilitation unit, and after rehabilitation 73 patients were discharged to their homes. Conclusions - Inpatient rehabilitation treatment could be necessary after operation of patients with brain tumor especially when functional disorders (disability) are present. Consultation is obligatory among the neurosurgeon, rehabilitation physician and the patient to set realistic rehabilitation goals and determine place and method of rehabilitation treatment, but even at malignancies cooperation with oncological specialist also needed. Authors’ experience shows benefits of multidisciplinary rehabilitation for patients after brain tumor surgery. ]
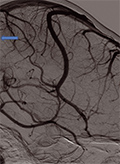
[Sturge Weber type 3 presenting with occipital epileptic seizure: case report ]
[Sturge Weber syndrome is the third most common neurocutaneous syndrome after neurofibromatosis and tuberous sclerosis. Three distinct types were identified. Type 3 with leptomeningeal involvement alone is the rarest among other types. The reported case is a 21-years-old female patient without any known chronic disease. She admitted to the emergency department after visual symptoms and headache, followed by generalized tonic clonic seizure. EEG of the patient showed left occipital seizure activity. The contrast enhanced magnetic resonance imaging (MRI) showed left occipital leptomeningeal angioma. Digital substraction angiography (DSA) revealed minimal blushed contrast enhancement on late venous phase and lack of superficial cortical veins. Her focal seizures were under control with levatiracetam and lacosamide treatment. The reported case is unique because of the late onset presentation with focal seizure without mental retardation.]
[Symptomatic trigeminal autonomic cephalalgia without headache]
[We report the case of a 60-year-old man who exhibited trigeminal autonomic symptoms on his right side (numbness of the face, reddening of the eye, nasal congestion) occurring several times a day, for a maximum of 60 seconds, without any pain. The complaints were similar to trigeminal autonomic cephalalgia, just without any headache. Our 60-year-old male patient underwent a craniocervical MRI as part of his neurological workup, which revealed lesions indicative of demyelination. Further testing was guided (ophthalmological examination, VEP, CSF test) by the presumptive diagnosis of multiple sclerosis. It is likely that in his case the cause of these trigeminal and autonomic paroxysms is MS. Here we present an overview of the few cases we found in the literature, although we did not find any similar case reports. Perhaps the most interesting among these is one in which the author describes a family: a 54-year-old female exhibiting the autonomic characteristics of an episodic cluster headache, only without actual headache, her son, who had typical episodic cluster headaches with autonomic symptoms, and the woman’s father, whose short-term periorbital headaches were present without autonomic symptoms. We had not previously encountered a case of trigeminal autonomic cephalalgia without headache in our practice, nor have we had an MS patient exhibiting similar neurologic symptoms. The significance of our case lies in its uniqueness. ]
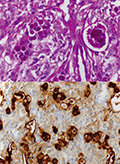
Secretory meningioma with bone infiltration and orbital spreading
Secretory meningioma is a rare form of meningiomas which differentiates from the meningothelial subtype. It is characterized by significant peritumor edema and distinct immunohistochemical and molecular genetic profiles. We present a middle aged female patient with secretory meningioma infiltrating the orbital bone from the primary cranial base location and causing exophthalmos, features rarely described with this tumor. Surgical resection was challenging because of the associated brain swelling and rich vascularization of the tumor. Imaging and immunohistochemical studies revealed characteristic hallmarks of secretory meningioma. While histologically it was a benign tumor, due to the orbital bone and soft tissue infiltration, postoperative management of neurological sequelae was challenging. This case highlights distinctive clinical, imaging and histological features along with individual characteristics of a rare form of meningiomas.
1.
Clinical Neuroscience
Is there any difference in mortality rates of atrial fibrillation detected before or after ischemic stroke?2.
Clinical Neuroscience
Factors influencing the level of stigma in Parkinson’s disease in western Turkey3.
Clinical Neuroscience
Neuropathic pain and mood disorders in earthquake survivors with peripheral nerve injuries4.
Journal of Nursing Theory and Practice
[Correlations of Sarcopenia, Frailty, Falls and Social Isolation – A Literature Review in the Light of Swedish Statistics]5.
Clinical Neuroscience
[Comparison of pain intensity measurements among patients with low-back pain]1.
2.
Clinical Neuroscience Proceedings
[A Magyar Stroke Társaság XVIII. Kongresszusa és a Magyar Neuroszonológiai Társaság XV. Konferenciája. Absztraktfüzet]3.
4.
Journal of Nursing Theory and Practice
[A selection of the entries submitted to the literary contest "Honorable mission: the joys and challenges of our profession" ]5.
Journal of Nursing Theory and Practice
[End of Life and Palliative Care of Newborns in the Nursing Context]