Posture correction as part of holistic health promotion in Hungarian schools
SOMHEGYI Annamária 1
MAY 30, 2022
Clinical Neuroscience - 2022;75(05-06)
DOI: https://doi.org/10.18071/isz.75.0151
Review
SOMHEGYI Annamária 1
MAY 30, 2022
Clinical Neuroscience - 2022;75(05-06)
DOI: https://doi.org/10.18071/isz.75.0151
Review
Szöveg nagyítása:
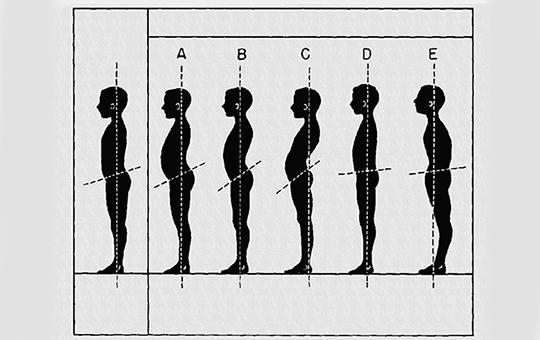
The primary prevention program of the Hungarian Spine Society was launched in 1995 with two goals: 1. to achieve that all school-children take part regularly in effective posture correcting exercises as part of physical education; and 2. to achieve daily physical education for all school-children. With appropriate governmental legislation and parliamentary decision both goals were integrated into the National Public Health Program in 2001 and 2003 and later in the national educational laws and documents. From 2011 and 2012 holistic health promotion in schools with the goal to reach all children became also prescription for all schools in Hungary. Public health institutions and actors still have to do much: they have to give continuous professional help to the physical education teachers in their posture correcting work and to all teachers in their daily health promoting tasks. The article presents the details of the special posture correcting exercises, their distribution and prospective controlled studies, their place in the national education, the present situation and the further tasks. The article is supplemented by a short report about daily physical education and holistic health promotion in schools: how the prescription was achieved, the essence and the follow up of it, and what are the tasks for the helping public health actors.
Clinical Neuroscience
We review the literature on REM parasomnias, and their the underlying mechanisms. Several REM parasomnias are consistent with sleep dissociations, where certain elements of the REM sleep pattern emerge in an inadequate time (sleep paralysis, hypnagogic hallucinations and cataplexy) or are absent/partial in their normal REM sleep time (REM sleep without atonia, underlying REM sleep behavior disorder). The rest of REM parasomnias (sleep related painful erection, catathrenia) may have other still unclear mechanisms. REM parasomnias deserve attention, because in addition to disturbing sleep and causing injuries, they may shed light on REM sleep functions as well as the heterogeneous etiologies of parasomnias. One of them, REM sleep behavior disorder has special importance as a warning sign of evolving neurodegenerative conditions mainly synucleinopathies (some cases synucleinopathies themselves) and it is a model parasomnia revealing that parasomnias may have by autoimmune, iatrogenic and even psychosomatic etiologies.
Clinical Neuroscience
Over the past year, many cases with newly onset or significantly exacerbated tic disorders were observed worldwide, where some aspects of the clinical presentation or the symptomatology were atypical for established tic diagnoses. Our purpose was to describe the atypical cases and raise relevant diagnostic issues. Consecutive cases with atypical tic presentations were documented. Five atypical tic cases are described. These cases shared some common characteristics, most notably the fact that all of them had been exposed to online presentation of ticking behaviour on social media platforms prior to the de novo development or exacerbation of their tics. Even though the order of events suggests causality and therefore the diagnosis of a functional tic disorder, unambiguous criteria for classifying atypical tics as functional symptoms are lacking. Differentiating neurodevelopmental and functional tics in childhood is currently problematic. Based on the currently unresolved issues in differential diagnosis, the importance of watchful waiting and behavioural interventions is highlighted to avoid unwarranted pharmacotherapy.
Clinical Neuroscience
Prevalence of acute ischemic stroke (AIS) is increased in patients with coronavirus disease 2019 (COVID-19). A proposed hypothesis is increased virus-induced propensity to hypercoagulation resulting in arterial thrombosis. Our aim was to provide evidence regarding the involvement of neutrophil extracellular trap (NET) formation (NETosis) in COVID-19 related AIS. Twenty-six consecutively enrolled COVID-19+ pneumonia patients with AIS, 32 COVID-19+ pneumonia patients without AIS and 24 AIS patients without COVID-19 infection were included to the study. Clinical characteristics of recruited patients were collected. Serum levels of citrullinated histone H3 (H3Cit; a factor of NETosis), IL-8 and C5a (mediators associated with NETosis) were measured by ELISA (enzyme-linked immunosorbent assay). H3Cit levels were significantly higher in COVID-19+ AIS patients, whereas all study groups showed comparable IL-8 and C5a levels. There were no significant differences among etiological subgroups of AIS patients with or without COVID-19. AIS patients with COVID-19 showed relatively increased white blood cell, lymphocyte, neutrophil, D-dimer, C-reactive protein and procalcitonin levels than control groups. H3Cit levels did not correlate with clinical/prognostic features and inflammation parameters. H3Cit and IL-8 levels were correlated in COVID-19 patients without stroke but not in COVID-19 positive or negative AIS patients. Increased levels of inflammation parameters and H3Cit in COVID-19 related AIS suggest that NETosis may cause susceptibility to arterial thrombosis. However, H3Cit levels do not correlate with clinical severity measures and inflammation parameters diminishing the prognostic biomarker value of NETosis factors. Moreover, the link between IL-8 and NETosis appears to be abolished in AIS.
Clinical Neuroscience
Neurological symptoms and complications associated with coronavirus 2019 (COVID-19) are well known. It was aimed to evaluate the brainstem and trigeminal/facial nerves and the pathways between these structures in COVID-19 using the blink reflex test. Thirty patients with post COVID-19 (16 males, 14 females) and 30 healthy individuals (17 males, 13 females) were included in this prospective study. Individuals who previously had a positive nose swap polymerase chain reaction test for severe acute respiratory syndrome coronavirus 2 and whose previously clinical features were compatible with COVID-19 were included in the post COVID-19 patient group. Neurological examination of the participants should be normal. Blink reflex test was performed on all participants. R1, ipsilateral R2 (IR2), and contralateral R2 (CR2) waves obtained from the test were analyzed. The mean ages of healthy individuals and post COVID-19 patients were 34.0±6.4 and 38.4±10.6 years, respectively. Both age and gender were matched between the groups. R1, IR2, and CR2 latencies/amplitudes were not different between the two groups. The side-to-side R1 latency difference was 0.5±0.3 and 1.0±0.8 ms in healthy individuals and post COVID-19 patients, respectively (p=0.011). One healthy individual and 12 patients with post COVID-19 had at least one abnormal blink reflex parameter (p=0.001). This study showed that COVID-19 may cause subclinical abnormalities in the blink reflex, which includes the trigeminal nerve, the seventh nerve, the brainstem, and pathways between these structures.
Clinical Neuroscience
Although severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) is a novel virus, many central and peripheral nervous system manifestations associated with coronavirus disease-19 (COVID-19) infection have been reported. Beyond the neurologic manifestations, we may still have much to learn about the neuropathologic mechanism of SARS-CoV-2 infection. Here we report a case of post-poliomyelitis syndrome (PPS) related to COVID-19 and attempt to predict the possible pathophysiologic mechanism behind this association.
Clinical Neuroscience
We aimed to investigate the association between fluoxetine use and the survival of hospitalised coronavirus disease (COVID-19) pneumonia patients. This retrospective case-control study used data extracted from the medical records of adult patients hospitalised with moderate or severe COVID-19 pneumonia at the Uzsoki Teaching Hospital of the Semmelweis University in Budapest, Hungary between 17 March and 22 April 2021. As a part of standard medical treatment, patients received anti-COVID-19 therapies as favipiravir, remdesivir, baricitinib or a combination of these drugs; and 110 of them received 20 mg fluoxetine capsules once daily as an adjuvant medication. Multivariable logistic regression was used to evaluate the association between fluoxetine use and mortality. For excluding a fluoxetine-selection bias potentially influencing our results, we compared baseline prognostic markers in the two groups treated versus not treated with fluoxetine. Out of the 269 participants, 205 (76.2%) survived and 64 (23.8%) died between days 2 and 28 after hospitalisation. Greater age (OR [95% CI] 1.08 [1.05–1.11], p<0.001), radiographic severity based on chest X-ray (OR [95% CI] 2.03 [1.27–3.25], p=0.003) and higher score of shortened National Early Warning Score (sNEWS) (OR [95% CI] 1.20 [1.01-1.43], p=0.04) were associated with higher mortality. Fluoxetine use was associated with an important (70%) decrease of mortality (OR [95% CI] 0.33 [0.16–0.68], p=0.002) compared to the non-fluoxetine group. Age, gender, LDH, CRP, and D-dimer levels, sNEWS, Chest X-ray score did not show statistical difference between the fluoxetine and non-fluoxetine groups supporting the reliability of our finding. Provisional to confirmation in randomised controlled studies, fluoxetine may be a potent treatment increasing the survival for COVID-19 pneumonia.
Clinical Neuroscience
[In this paper we present the Comprehensive Aphasia Test-Hungarian (CAT-H; Zakariás and Lukács, in preparation), an assessment tool newly adapted to Hungarian, currently under standardisation. The test is suitable for the assessment of an acquired language disorder, post-stroke aphasia. The aims of this paper are to present 1) the main characteristics of the test, its areas of application, and the process of the Hungarian adaptation and standardisation, 2) the first results from a sample of Hungarian people with aphasia and healthy controls. Ninety-nine people with aphasia, mostly with unilateral, left hemisphere stroke, and 19 neurologically intact control participants were administered the CAT-H. In addition, we developed a questionnaire assessing demographic and clinical information. The CAT-H consists of two parts, a Cognitive Screening Test and a Language Test. People with aphasia performed significantly worse than the control group in all language and almost all cognitive subtests of the CAT-H. Consistent with our expectations, the control group performed close to ceiling in all subtests, whereas people with aphasia exhibited great individual variability both in the language and the cognitive subtests. In addition, we found that age, time post-onset, and type of stroke were associated with cognitive and linguistic abilities measured by the CAT-H. Our results and our experiences clearly show that the CAT-H provides a comprehensive profile of a person’s impaired and intact language abilities and can be used to monitor language recovery as well as to screen for basic cognitive deficits in aphasia. We hope that the CAT-H will be a unique resource for rehabilitation professionals and aphasia researchers in aphasia assessment and diagnostics in Hungary. ]
Clinical Neuroscience
[The well-known gap between stroke mortality of Eastern and Western European countries may reflect the effect of socioeconomic differences. Such a gap may be present between neighborhoods of different wealth within one city. We set forth to compare age distribution, incidence, case fatality, mortality, and risk factor profile of stroke patients of the poorest (District 8) and wealthiest (District 12) districts of Budapest. We synthesize the results of our former comparative epidemiological investigations focusing on the association of socioeconomic background and features of stroke in two districts of the capital city of Hungary. The “Budapest District 8–12 project” pointed out the younger age of stroke patients of the poorer district, and established that the prevalence of smoking, alcohol-consumption, and untreated hypertension is also higher in District 8. The “Six Years in Two Districts” project involving 4779 patients with a 10-year follow-up revealed higher incidence, case fatality and mortality of stroke in the less wealthy district. The younger patients of the poorer region show higher risk-factor prevalence, die younger and their fatality grows faster during long-term follow-up. The higher prevalence of risk factors and the higher fatality of the younger age groups in the socioeconomically deprived district reflect the higher vulnerability of the population in District 8. The missing link between poverty and stroke outcome seems to be lifestyle risk-factors and lack of adherence to primary preventive efforts. Public health campaigns on stroke prevention should focus on the young generation of socioeconomically deprived neighborhoods. ]
Clinical Neuroscience
Microdiscectomy (MD) is a standard technique for the surgical treatment of lumbar disc herniation (LDH). Uniportal percutaneous full-endoscopic interlaminar lumbar discectomy (PELD) is another surgical option that has become popular owing to reports of shorter hospitalization and earlier functional recovery. There are very few articles analyzing the total costs of these two techniques. The purpose of this study was to compare total hospital costs among microdiscectomy (MD) and uniportal percutaneous full-endoscopic interlaminar lumbar discectomy (PELD). Forty patients aged between 22-70 years who underwent PELD or MD with different anesthesia techniques were divided into four groups: (i) PELD-local anesthesia (PELD-Local) (n=10), (ii) PELD-general anesthesia (PELD-General) (n=10), (iii) MD-spinal anesthesia (MD-Spinal) (n=10), (iv) MD-general anesthesia (MD-General) (n=10). Health care costs were defined as the sum of direct costs. Data were then analyzed based on anesthetic modality to produce a direct cost evaluation. Direct costs were compared statistically between MD and PELD groups. The sum of total costs was $1,249.50 in the PELD-Local group, $1,741.50 in the PELD-General group, $2,015.60 in the MD-Spinal group, and $2,348.70 in the MD-General group. The sum of total costs was higher in the MD-Spinal and MD-General groups than in the PELD-Local and PELD-General groups. The costs of surgical operation, surgical equipment, anesthesia (anesthetist’s costs), hospital stay, anesthetic drugs and materials, laboratory workup, nursing care, and postoperative medication differed significantly among the two main groups (PELD-MD) (p<0.01). This study demonstrated that PELD is less costly than MD.
1.
Clinical Neuroscience
[Headache registry in Szeged: Experiences regarding to migraine patients]2.
Clinical Neuroscience
[The new target population of stroke awareness campaign: Kindergarten students ]3.
Clinical Neuroscience
Is there any difference in mortality rates of atrial fibrillation detected before or after ischemic stroke?4.
Clinical Neuroscience
Factors influencing the level of stigma in Parkinson’s disease in western Turkey5.
Clinical Neuroscience
[The effects of demographic and clinical factors on the severity of poststroke aphasia]1.
2.
Clinical Oncology
[Pancreatic cancer: ESMO Clinical Practice Guideline for diagnosis, treatment and follow-up]3.
Clinical Oncology
[Pharmacovigilance landscape – Lessons from the past and opportunities for future]4.
5.
COMMENTS
0 comments