The eLitMed.hu medical portal uses computer cookies for convenient operation. Detailed information can be found in the Cookie-policy.
Hungarian Immunology - 2004;3(01)
Content
[Gene therapy as a treatment for rheumatoid arthritis]
[A clear understanding of the pathogenic events and/or environmental conditions that lead to the development of rheumatoid arthritis has not been accomplished. In recent years, some of the most capable therapies have targeted individual proteins, such as proinflammatory cytokines, which contribute to persistent inflammation. The success of these therapies in some patients underscores the importance of having a solid pathophysiologic knowledge of the mechanisms at play in the diseased joint. Targeting the joint therapeutically with proteins or other agents has presented many challenges in the treatment of rheumatoid arthritis. To circumvent these obstacles, the idea of providing transgenes to cells of the synovial lining was born. This use of gene therapy, as a delivery vehicle rather than replacement of a genetic deficit, has had many successes in preclinical animal studies. Preliminary results of the first Phase I clinical trial in humans suggests that an ex vivo approach can be safe and enable transgene expression. This review provides a consolidated overview of many of the successful gene therapy strategies undertaken for the treatment of animal models of arthritis. The focus is on: 1. joint targeting strategies, including discussion on the local and systemic approaches as well as the contralateral joint; 2. the applicability of viral vectors, including comparison of adenoviral, retroviral, adeno-associated, and herpes simplex viruses; 3. timing and dosage of treatment; and 4. targets and candidate proteins that have been examined, including targeting proinflammatory cytokines or the use of anti-inflammatory cytokines.]
[TNF-α blocking therapy in rheumatoid arthritis]
[The research of pathomechanism of rheumatoid arthritis resulted in remarkable pragmatic results beyond the important theoretical knowledge. These observations led to the development of new effective agents, which were named as biological therapy and introduced in clinical praxis. The key factor of pathomechanism of rheumatoid arthritis is the proinflammatoric citokin TNF-α. It can be found on the top of the inflammation cascade where regulates many other inflammatory mediators and also plays an important role in the defence against infections and tumours. The author describes the TNF-α blocking agents used in clinical practice, their chemical and pharmacological feature, as well as their mode of action and the consequence of inhibition of TNF-α. He reviews the main results of the major clinical tests with infliximab, etanercet, and adalimumab. The results of these clinical studies demonstrate that the TNF-α blocking therapy gives clinical improvement in case of therapy resistant patients, decreases the number of swollen and tender joints, the pain, ESR and CRP, decreases the radiological progression, furthermore improves the quality of life. There are also some data about the favourable impacts observed during the early arthritis treatment. The TNF-α blocking therapy can be used effectively and safely in rheumatoid arthritis. In most cases the infusion reaction and the injection site reaction are not reasons for withdrawal from the study. The sideeffects, however, developed in increasing numbers during widespread applications. Among these the most important ones are the opportunist infection and the tuberculosis. In addition the sporadic occurrence of lupus-like symptoms, demyelinating disease, and aplastic anemia were reported. The fundamental requirements of the safety of the biological therapy are the professional indication and the careful monitoring during the treatment, the principle of which has been already prepared by the Professional College of the Rheumatology and Physiotherapy based on the international experience.]
[Experience with infliximab treatment of rheumatoid arthritis in Hungary]
[We conducted the first Hungarian open-label study using infliximab (Remicade) in 62 rheumatoid arthritis (RA) patients. The mean disease duration was 8.7 years. Patients receiving methotrexate for at least 3 months with active RA were included in the study. All patients received concomittant methotrexate treatment. Results indicated a 61%, 35% and 18% improvement in ACR20, ACR50 and ACR70, respectively. In most patients, dramatic improvement was seen as soon as after the first or second infusion.]
[Intracytoplasmic cytokines in dermatomyositis]
[OBJECTIVE - To investigate the intracellular and soluble cytokine levels in peripheral blood of patients with active and inactive dermatomyositis (DM). Methods The frequency of the intracellular IFN-g, IL- 4 and IL-10 expression of CD4+ or CD8+ cells were determined by flow cytometry. We measured the concentrations of soluble cytokines with commercial ELISAs. RESULTS - In active DM we observed decreased IFNg expression of CD4+ and CD8+ cells. These prominent changes disappeared in the inactive stage of the disease. In DM we could not detect a significant change in the intracellular IL-4 cytokine expression either in the active or in the inactive form. The IL-10 expression was elevated in the inactive state of the patients. CONCLUSION - We can state that a difference between aDM and iDM seems to exist in the level of peripheral blood lymphocytes and their intracellular cytokine content.]
[Cyclosporin A therapy of autoimmune urticaria]
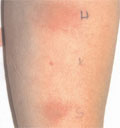
[INTRODUCTION - In chronic idiopathic urticaria the etiology is unknown in spite of extensive investigations. In 27-50% of these cases autoimmune mechanisms are detected in the background. CASE REPORT - The authors demonstrate the case of an autoimmune urticaria patient with positive autologous serum skintest, who responded well to cyclosporin A therapy. CONCLUSION - According to the observation and the relevant literature, the authors also found small dose cyclosporin A therapy useful and safe in treating therapy resistant chronic urticaria.]
1.
Clinical Neuroscience
[Headache registry in Szeged: Experiences regarding to migraine patients]2.
Clinical Neuroscience
[The new target population of stroke awareness campaign: Kindergarten students ]3.
Clinical Neuroscience
Is there any difference in mortality rates of atrial fibrillation detected before or after ischemic stroke?4.
Clinical Neuroscience
Factors influencing the level of stigma in Parkinson’s disease in western Turkey5.
Clinical Neuroscience
[The effects of demographic and clinical factors on the severity of poststroke aphasia]1.
2.
Clinical Oncology
[Pancreatic cancer: ESMO Clinical Practice Guideline for diagnosis, treatment and follow-up]3.
Clinical Oncology
[Pharmacovigilance landscape – Lessons from the past and opportunities for future]4.
5.