The eLitMed.hu medical portal uses computer cookies for convenient operation. Detailed information can be found in the Cookie-policy.
Specialities
Endocrinology
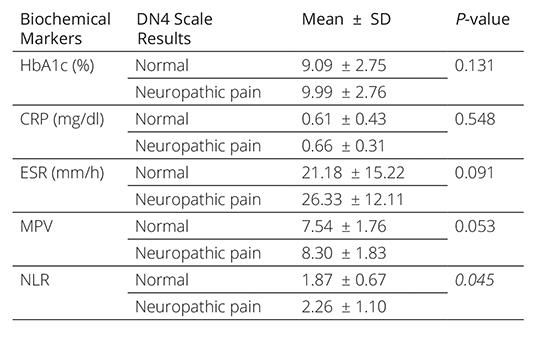
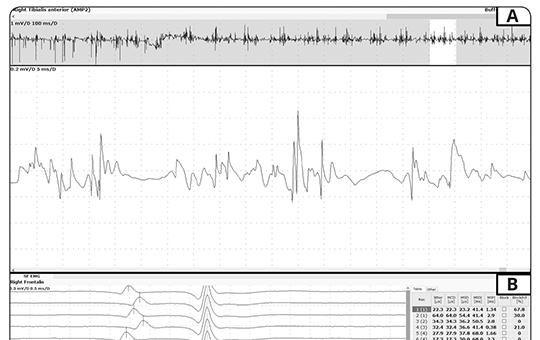
The significance of neutrophil/lympocyte ratio and platelet/lymphocyte ratio in predicting diabetic polyneuropathy and neuropathic pain severity as inflammatory factors
Neuropathic pain may appear as one of the first symptoms that take the patient to the physician in type 2 diabetes, which can be asymptomatic for years. Although it is accepted that diabetes is a trigger for vascular inflammation, it has been suggested that inflammation itself may trigger diabetes. In our study, we aimed to investigate the relationship between diabetic polyneuropathy and neuropathic pain and inflammatory markers.
Pembrolizumab-induced peripheral nervous system damage: A combination of myositis/ myasthenia overlap syndrome and motor axonal polyneuropathy
Immune-checkpoint inhibitors (ICI) are effective drugs in cancer treatment that block immune checkpoints and stimulate an attack on cancer cells. However, various side effects were reported with ICIs. Peripheral nervous system (PNS) side effects are three times more frequent than those in the central nervous system. A 63-year-old male patient was admitted to our department with a 10-day history of dyspnea, diplopia, and generalized weakness.
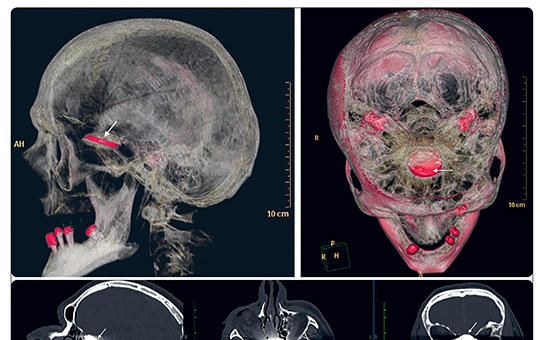
Minimal invasive transnasal endoscopic removal of intracranial foreign body after airbag deployment
Airbag induced injuries such as skull and cervical spine fractures, epidural and subdural hematomas, atlantooccipital dislocations or brainstem lacerations are already documented in published literature, however, no previous case have been published about a penetrating foreign body of the skull base following airbag deployment. Removal of an intracranial foreign body is very dangerous and difficult.
[Disturbances of lipid metabolism in endocrine disorders ]
[Dyslipidemia plays a crucial role in the pathogenesis of several cardiovascular diseases. In many patients, there is no primary disorder of the lipoprotein metabolism since the condition is caused by whichever “nonlipid” etiology. These secondary dyslipidemias are surprisingly common, and their background factors are often missed if they are not scrutinized systematically. Endocrine disorders are commonly associated with dyslipidemia, including hypothyroidism, diabetes mellitus, Cushing’s syndrome, acromegaly, hypogonadism, growth hormone deficiency, hyperprolactinemia, and polycystic ovary syndrome. Recognizing these conditions is essential since the lipid abnormalities respond well to the treatment of primary disorders in most cases. Thus diagnosing the endocrine diseases during the routine investigation of dyslipidemia patients is essential for effective treatment and prevention of cardiovascular diseases.]
[High blood pressure and low testosterone levels both increase the risk of cardiovascular disease and alter the morphology and function of blood vessels]
[Both hypertension and andropause alone increase the risk of cardiovascular disease. The incidence of both diseases increases with age. As a consequence they may often present concurrently in men. The damaging effects of the two noxae may add up - this may be observed in the remodeling processes of coronary resistance vessels. This mini-review summarizes the effects of hipertension, testosterone deficiency and the combined effects of these two noxae on the morphological, biomechanical and functional adaptation of coronary resistance vessels, as well as on cardiovascular diseases.]
[Is hypertension different for women and men?]
[Hypertension is a risk factor for cardiovascular diseases in both men and women. Lifelong studies have proven that women suffer from high blood pressure in old age more often than men and this is often associated with obesity, dyslipidemia, and diabetes. All of this can most likely be related to menopause, when one of the most important female sex hormones, estrogen’s vascular protective and anti-inflammatory effect ceases. It has also been proven that pregnancy is also a test for the vascular system. Pathological abnormalities during pregnancy increase the cardiovascular risk later on. Differences can be detected in the regulation of blood pressure, as a result of the autonomic nervous system and hormonal effects. Differences can also be discovered in relation to common cardiovascular diseases. Although the recommendations do not currently differentiate, the effectiveness of the therapies and the frequency of side effects may also differ. Recent researches conclude that women’s cardiovascular risk is manifested in lower blood pressure values than men’s. It is possible that we should modify the threshold and target values of women’s blood pressure in order to decrease the proven cardiovascular risk of high blood pressure in women through well-planned therapy.]
1.
Clinical Neuroscience
[Headache registry in Szeged: Experiences regarding to migraine patients]2.
Clinical Neuroscience
[The new target population of stroke awareness campaign: Kindergarten students ]3.
Clinical Neuroscience
Is there any difference in mortality rates of atrial fibrillation detected before or after ischemic stroke?4.
Clinical Neuroscience
Factors influencing the level of stigma in Parkinson’s disease in western Turkey5.
Clinical Neuroscience
[The effects of demographic and clinical factors on the severity of poststroke aphasia]1.
2.
Clinical Oncology
[Pancreatic cancer: ESMO Clinical Practice Guideline for diagnosis, treatment and follow-up]3.
Clinical Oncology
[Pharmacovigilance landscape – Lessons from the past and opportunities for future]4.
5.