The eLitMed.hu medical portal uses computer cookies for convenient operation. Detailed information can be found in the Cookie-policy.
Hungarian Immunology - 2004;3(04)
Content
[Therapeutic treatment of rheumatoid arthritis by gene therapy-induced apoptosis]
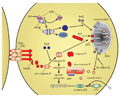
[Gene therapy was initially conceptualized as a treatment for individuals with genetic disorders, where defective genes would be replaced with functional ones. This concept was eventually broadened to include the use of gene therapy as a delivery mechanism for gene products effective in the treatment of diseases. The latter use of gene therapy, essentially as a drug delivery mechanism, was recognized to be particularly useful in the treatment of rheumatoid arthritis because it may have many advantages over traditional therapies. Two groups of target genes that are potentially useful for gene transfer include soluble inflammatory mediators that in theory could suppress the inflammatory process, and apoptotic mediators that may induce cell death, thereby suppressing the accumulation of inflammatory cells in the joint. To date the former group of target genes has received most of the attention, but it is the latter group of apoptosis-inducing targets that will be discussed in this review. We will focus our discussion on target genes that have shown success at inducing apoptosis in animal models of arthritis and will also include discussion of the apoptotic pathways that are altered in the attempts to reduce inflamed synovial tissue.]
[Changes of immune system in the elderly]
[”Immunosenescence” means the change of the immune system with ageing. Ageing of the immun system is a physiological process, based on complex immunregulatory alterations, which make the elderly more susceptible for infections, malignant and autoimmun diseases. It’s important to differentiate the primary (physiological) and secondory (caused by diseases) modifications of immunregulatory system. After reviewing the strict Senieur protocoll, which makes a basis for gerontological/geriatry studies, the authors survey in details the changes of the each cell types of the immune system. The impaired functions of the NK (natural killer) and PMN (polymorphonuclear) cells and macrophags (as the parts of innate immunity), the decreased numbers of T lymphocyts, and the less specific antibodies produced by B lymphocyts (as the part of the acquired immunity) together are responsible for the increased susceptibility of the elderly to infections, and for the higher prevalence of malignancies in elderly patients. The imbalance of pro- and anti-inflammatoric cytokines and the TH1- TH2 shift also play role in this process. Appearance of autoantigens and the increased autoreactivity are in the background of the frequency autoimmun diseases in the elderly. The development of malignant diseases is a complex process, caused by on the one hand the changes in innate immunity, on the other the decreased activity of suppressor mechanisms. These changes are not correctly known, but the literature grows increasingly. The good command of the molecular mechanisms provides the facilities to improve remedial interventions in the future.]
[Immunology of Felty’s syndrome]
[Felty’s syndrome can be regarded as “super-rheumatoid” disease. Immungenetically the syndrome is much more homogenous, than rheumatoid arthritis. HLA-DRB1*0401 antigen is present in 83% of the patients. Felty’s syndrome develops usually after a longer course of rheumatoid arthritis, in 1% of rheumatoid patients. Rheumatoid arthritis patients with long lasting unexplained neutropenia can be diagnosed having Felty’s syndrome, even without detectable splenomegaly. On the contrary, rheumatoid arthritis with splenomegaly, but without present or previous neutropenia with unexplained origin cannot be regarded as having Felty’s syndrome. Inspite of the fact, that the arthritis of Felty’s syndrome can be inactive, because of the neutropenia and increased risk of recurrent infections, the patients should be kept under tight supervision, and should be properly treated, if required. Immunologically Felty’s syndrome is characterized by rheumatoid factor positivity in 95-100%, ANA positivity in 50-100%, antihistone positivity in 63-83%. Antibodies against dsDNA rarely, but against ssDNA frequently occur. No anti Sm and interestingly no anti Ro and anti La antibodies can be detected inspite of the high incidence of associated Sjögren’s syndrome. Immunoglobulin levels are higher and complement levels are lower, than in rheumatoid arthritis. Circulating immuncomplex level is usually high. Non-specific antineutrophil anticitoplasmatic antibodies can be found in high percentage. The neutropenia of Felty’s syndrome can be either caused by increased IgG neutrophilic binding activity or by inhibition of the granulocytes colony growing in the bone marrow, by peripheral blood mononuclear cells. Expansion of large granular lymphocytes can be seen in 30-40% of patients with Felty’s syndrome. Large granular lymphocyte syndrome is not rarely associated with rheumatoid arthritis. The neutrophil account is normal or elevated in this syndrome, but splenomegaly occurs. These cases are called as pseudo Felty’s syndrome. The patients with Felty's syndrome suffering from recurrent infections required treatment even if the arthritis is inactive. Methotrexate treatment should be started first, if this treatment fails, other disease modifying drugs or colony stimulating factor can be given. There is no experience with other biological treatments. In treatment of resistant cases splenectomy is indicated. Non-steroid anti-inflammatory drugs should be better avoided.]
[Investigation of activated T-cells by non-Hodgkin’s lymphoma patients]
[BACKGROUND - The immune system has several mechanisms to fight against developing malignant cell clones in the host, one of them is the activated T-cell response. Both CD4+ helper and CD8+ cytotoxic T-cells bear CD69 and HLA-DR molecules as important surface activation markers. AIM - Our aim was to determine, how the ratio of activated T-cells change in the peripheral blood of non-Hodgkin-lymphoma patients during the periods of polychemotherapy. PATIENTS AND METHODS - We used the peripheral blood samples of 43 non-Hodgkin-lymphoma’s patients (20 females, 23 males, mean age 52.4 years). We determined the level of CD3+/HLADR+ and CD3+/CD69+ T-cell subsets before, during and after the periods of polychemotherapy, using the methods of immunofluorescence stain and flow cytometry. RESULTS - We found the ratio of CD3+/HLA-DR+ cells significantly higher in non-Hodgkin-lymphoma’s patients before treatment compared to healthy controls (10.63% vs. 2.97%, p<0.001). During the period of polychemotherapy, this ratio began to increase significantly (16.94% vs. 10.63%, p=0.006). The level of CD3+/CD69+ cells did not change significantly. After treatment, the ratio of activated T-cells decreased, however, we detected significantly higher rate of CD3+/HLA-DR+ lymphocytes in patients who relapsed within one year than in those who stayed in remission (9.55% vs. 20.62%, p<0.001). CONCLUSION - Investigation of CD3+/HLA-DR+ activated T-cells might be a promising method to determine the immune defence and this way the prognostics of lymphoma patients.]
1.
Clinical Neuroscience
[Headache registry in Szeged: Experiences regarding to migraine patients]2.
Clinical Neuroscience
[The new target population of stroke awareness campaign: Kindergarten students ]3.
Clinical Neuroscience
Is there any difference in mortality rates of atrial fibrillation detected before or after ischemic stroke?4.
Clinical Neuroscience
Factors influencing the level of stigma in Parkinson’s disease in western Turkey5.
Clinical Neuroscience
[The effects of demographic and clinical factors on the severity of poststroke aphasia]1.
2.
Clinical Oncology
[Pancreatic cancer: ESMO Clinical Practice Guideline for diagnosis, treatment and follow-up]3.
Clinical Oncology
[Pharmacovigilance landscape – Lessons from the past and opportunities for future]4.
5.