The eLitMed.hu medical portal uses computer cookies for convenient operation. Detailed information can be found in the Cookie-policy.
Clinical Neuroscience - 2020;73(07-08)
Content
[Decisional collisions between evidence and experience based medicine in care of people with epilepsy]
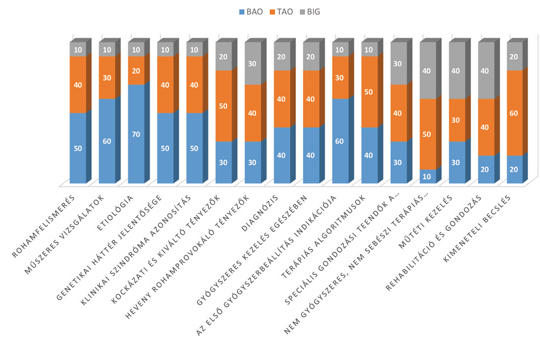
[Background – Based on the literature and his long-term clinical practice the author stresses the main collisions of evidence and experience based medicine in the care of people with epilepsy. Purpose – To see, what are the professional decisions of high responsibility in the epilepsy-care, in whose the relevant clinical research is still lacking or does not give a satisfactory basis. Methods – Following the structure of the Hungarian Guideline the author points the critical situations and decisions. He explains also the causes of the dilemmas: the lack or uncertainty of evidences or the difficulty of scientific investigation of the situation. Results – There are some priorities of experience based medicine in the following areas: definition of epilepsy, classification of seizures, etiology – including genetic background –, role of precipitating and provoking factors. These are able to influence the complex diagnosis. In the pharmacotherapy the choice of the first drug and the optimal algorithm as well as the tasks during the care are also depends on personal experiences sometimes contradictory to the official recommendations. Same can occur in the choice of the non-pharmacological treatments and rehabilitation. Discussion and conclusion – Personal professional experiences (and interests of patients) must be obligatory accessories of evidence based attitude, but for achieving the optimal results, in some situations they replace the official recommendations. Therefore it is very important that the problematic patients do meet experts having necessary experiences and also professional responsibility to help in these decisions. ]
[Comparative analysis of the full and shortened versions of the Oldenburg Burnout Inventory]
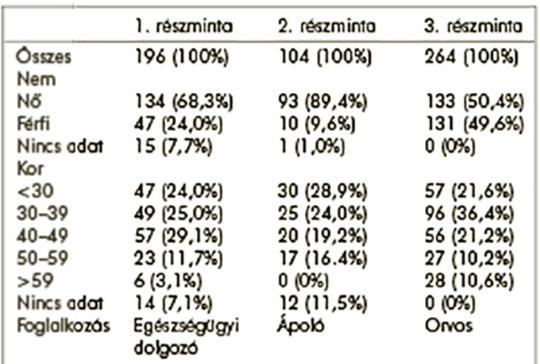
[Background – The two free-to-use versions of the Oldenburg Burnout Inventory (OLBI) have been increasingly utilised to assess the prevalence of burnout among human service workers. The OLBI has been developed to overcome some of the psychometric and conceptual limitations of the Maslach Burnout Inventory, the gold standard of burnout measures. There is a lack of data on the structural validity of the Mini Oldenburg Burnout Inventory and the Oldenburg Burnout Inventory in Hungary. Purpose – To assess the structural validity of the Hungarian versions of the Oldenburg Burnout Inventory and the Mini-Oldenburg Burnout Inventory. Methods – We enrolled 564 participants (196 healthcare workers, 104 nurses and 264 clinicians) in three cross-sectional surveys. In our analysis we assessed the construct validity of the instruments using confirmatory factor analysis and internal consistency using coefficient Cronbach’s α. Results – We confirmed the two-dimensional structure (exhaustion and disengagement) of the Mini-Oldenburg Inventory and a shortened version of the Oldenburg Burnout Inventory Internal consistency coefficient confirmed the reliability of the instruments. The burnout appeared more than a 50 percent of the participants in every subsample. The prevalence of exhaustion was above 54.5% in each of the subsamples and the proportion of disengaged clinicians was particularly high (92%). Conclusions – Our findings provide support for the construct validity and reliability of the Hungarian versions of the Mini-Oldenburg Burnout Inventory and a shortened version of the Oldenburg Burnout Inventory in the assessment of burnout among clinicians and nurses in Hungary.]
[What happens to vertiginous population after emission from the Emergency Department?]
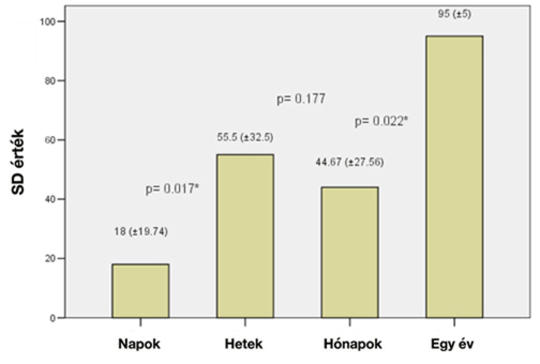
[Background – Dizziness is one of the most frequent complaints when a patient is searching for medical care and resolution. This can be a problematic presentation in the emergency department, both from a diagnostic and a management standpoint. Purpose – The aim of our study is to clarify what happens to patients after leaving the emergency department. Methods – 879 patients were examined at the Semmelweis University Emergency Department with vertigo and dizziness. We sent a questionnaire to these patients and we had 308 completed papers back (110 male, 198 female patients, mean age 61.8 ± 12.31 SD), which we further analyzed. Results – Based on the emergency department diagnosis we had the following results: central vestibular lesion (n = 71), dizziness or giddiness (n = 64) and BPPV (n = 51) were among the most frequent diagnosis. Clarification of the final post-examination diagnosis took several days (28.8%), and weeks (24.2%). It was also noticed that 24.02% of this population never received a proper diagnosis. Among the population only 80 patients (25.8%) got proper diagnosis of their complaints, which was supported by qualitative statistical analysis (Cohen Kappa test) result (κ = 0.560). Discussion – The correlation between our emergency department diagnosis and final diagnosis given to patients is low, a phenomenon that is also observable in other countries. Therefore, patient follow-up is an important issue, including the importance of neurotology and possibly neurological examination. Conclusion – Emergency diagnosis of vertigo is a great challenge, but despite of difficulties the targeted and quick case history and exact examination can evaluate the central or peripheral cause of the balance disorder. Therefore, to prevent declination of the quality of life the importance of further investigation is high.]
[Recurrent inhibition during Jendrassik maneuver]
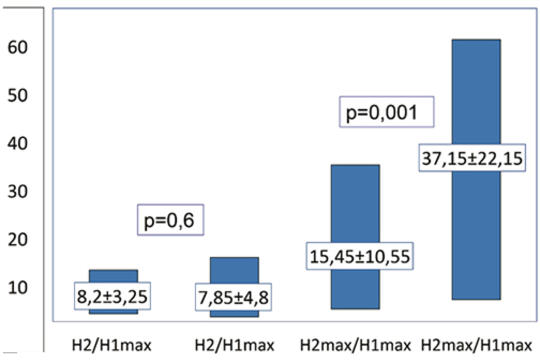
[Objective – Conflicting theoretical models exist regarding the mechanism related to the ability of the Jendrassik maneuver to reinforce reflex parameters. Our objective was to investigate if vigorous handgrip would induce changes in recurrent inhibition of soleus motoneurons. Method – Soleus H reflex was evoked by stimulating the tibial nerve at rest and during bilateral vigorous handgrip, alternating single (H1) and paired stimulation (H2). At paired stimulation we used interstimulus intervals of 10, 15, 20 and 25 ms and supramaximal test stimulus. H1- and H2-wave amplitudes were expressed as percentage of maximal M-wave amplitude. Conditioned H2 wave maximal (H2max) and minimal (H2) amplitudes evoked at rest and expressed as a percentage of the unconditioned H1max amplitude were compared with the corresponding values obtained during handgrip by means of paired Student test and Bonferroni correction. Subjects – At the study participated 28 healthy volunteers. Results – The H1max/Mmax × 100 values obtained during handgrip (37.5±10.1) were significantly higher than those obtained at rest (27.1±7.4). The H2max/H1max × 100-values obtained at paired stimulation were significantly higher during handgrip than at rest, while no significant difference was found between the H2/H1max × 100-values obtained during handgrip and at rest respectively. Discussion – The H2max/H1max is determined by both the excitability of the motoneurons and the recurrent inhibition elicited by the conditioning stimulus, while H2/H1max indicates only the level of recurrent inhibition. According to our results the Renshaw cells retain their inhibitory effect on the soleus alpha motoneurons during remote muscle contraction. Conclusion – Soleus H reflex enhancement during Jendrassik maneuver is not due to decrease of recurrent inhibition. ]
[Objective measurement of manual dexterity of Parkinson patients operated with DBS]
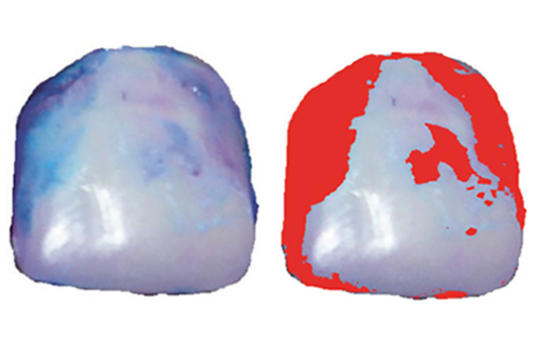
[The evaluation of hand dexterity is an important marker for the success of DBS (deep brain stimulation) operation in patients with Parkinson’s disease. In this study we applied a simple, semiquantitative optical dental plaque staining technique for the evaluation of the hand dexterity. Ten patient with Parkinson’s disease were involved in the study. After dental students aided tooth brushing, bacterial dental deposits (plaque) were stained then photographed, and quantified under standard conditions before and after DBS surgery. Our results showed a significant decrease in dental plaque deposits after DBS operation. This simple technique seems to be a routinely applicable marker for the evaluation of the hand dexterity. Our future plans is repeating the previous experiement on a higher number of cases.]
[Advanced Parkinson’s disease characteristics in clinical practice: Results from the OBSERVE-PD study and sub-analysis of the Hungarian data]
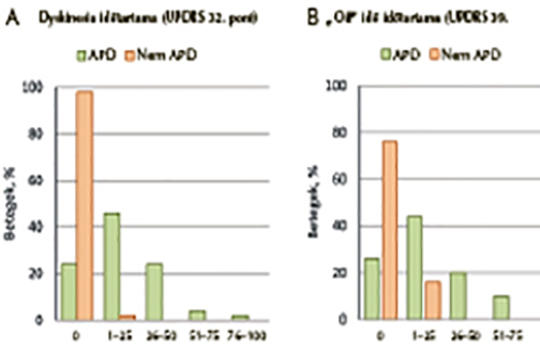
[The majority of patients with advanced Parkinson’s disease are treated at specialized movement disorder centers. Currently, there is no clear consensus on how to define the stages of Parkinson’s disease; the proportion of Parkinson’s patients with advanced Parkinson’s disease, the referral process, and the clinical features used to characterize advanced Parkinson’s disease are not well delineated. The primary objective of this observational study was to evaluate the proportion of Parkinson’s patients identified as advanced patients according to physician’s judgment in all participating movement disorder centers across the study. Here we evaluate the Hungarian subset of the participating patients. The study was conducted in a cross-sectional, non-interventional, multi-country, multi-center format in 18 countries. Data were collected during a single patient visit. Current Parkinson’s disease status was assessed with Unified Parkinson’s Disease Rating Scale (UPDRS) parts II, III, IV, and V (modified Hoehn and Yahr staging). Non-motor symptoms were assessed using the PD Non-motor Symptoms Scale (NMSS); quality of life was assessed with the PD 8-item Quality-of-Life Questionnaire (PDQ-8). Parkinson’s disease was classified as advanced versus non-advanced based on physician assessment and on questions developed by the Delphi method. Overall, 2627 patients with Parkinson’s disease from 126 sites were documented. In Hungary, 100 patients with Parkinson’s disease were documented in four movement disorder centers, and, according to the physician assessment, 50% of these patients had advanced Parkinson’s disease. Their mean scores showed significantly higher impairment in those with, versus without advanced Parkinson’s disease: UPDRS II (14.1 vs. 9.2), UPDRS IV Q32 (1.1 vs. 0.0) and Q39 (1.1 vs. 0.5), UPDRS V (2.8 vs. 2.0) and PDQ-8 (29.1 vs. 18.9). Physicians in Hungarian movement disorder centers assessed that half of the Parkinson’s patients had advanced disease, with worse motor and non-motor symptom severity and worse QoL than those without advanced Parkinson’s disease. Despite being classified as eligible for invasive/device-aided treatment, that treatment had not been initiated in 25% of these patients.]
[The complex intensive care and rehabilitation of a quadriplegic patient using a diaphragm pacemaker]
[A 21 year female polytraumatized patient was admitted to our unit after a serious motorbike accident. We carried out CT imaging, which confirmed the fracture of the C-II vertebra and compression of spinal cord. Futhermore, the diagnostic investigations detected the compound and comminuted fracture of the left humerus and femur; the sacrum and the pubic bones were broken as well. After the stabilization of the cervical vertebra, a tracheotomy and the fixation of her limbs were performed. She spent 1.5 years in our unit. Meanwhile we tried to fix all the medical problems related to tetraplegia and respiratory insufficiency. As part of this process she underwent an electrophysiological examination in Uppsala (Sweden) and a diaphragm pacemaker was implanted. Our main goal was to reach the fully available quality of life. It is worth making this case familiar in a wider range of public as it could be an excellent example for the close collaboration of medical and non-medical fields.]
Life threatening rare lymphomas presenting as longitudinally extensive transverse myelitis: a diagnostic challenge
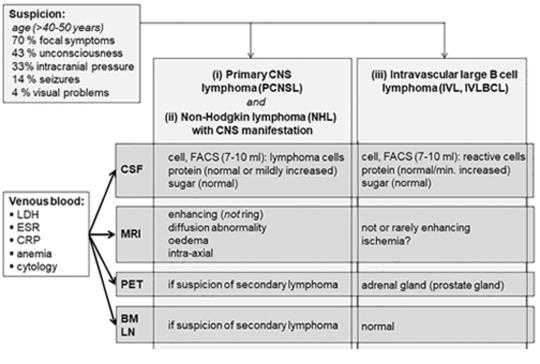
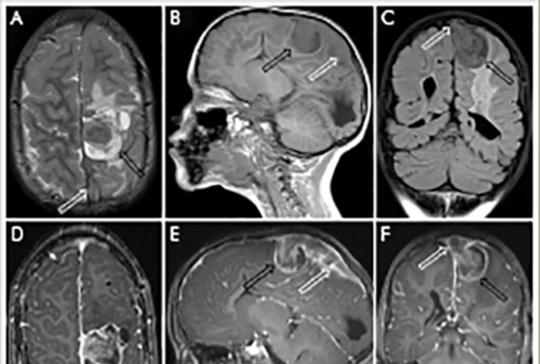
Background and aims – Description of two cases of rare intravascular large B-cell lymphoma and secondary T-cell lymphoma diagnosed postmortem, that manifested clinically as longitudinally extensive transverse myelitis (LETM). We discuss causes of diagnostic difficulties, deceptive radiological and histological investigations, and outline diagnostic procedures based on our and previously reported cases. Case reports – Our first case, a 48-year-old female was admitted to the neurological department due to paraparesis. MRI suggested LETM, but the treatments were ineffective. She died after four weeks because of pneumonia and untreatable polyserositis. Pathological examination revealed intravascular large B-cell lymphoma (IVL). Our second case, a 61-year-old man presented with headache and paraparesis. MRI showed small bitemporal lesions and lesions suggesting LETM. Diagnostic investigations were unsuccessful, including tests for possible lymphoma (CSF flow cytometry and muscle biopsy for suspected IVL). Chest CT showed focal inflammation in a small area of the lung, and adrenal adenoma. Brain biopsy sample from the affected temporal area suggested T-cell mediated lymphocytic (paraneoplastic or viral) meningoencephalitis and excluded diffuse large B-cell lymphoma. The symptoms worsened, and the patient died in the sixth week of disease. The pathological examination of the presumed adenoma in the adrenal gland, the pancreatic tail and the lung lesions revealed peripheral T-cell lymphoma, as did the brain and spinal cord lesions. Even at histological examination, the T-cell lymphoma had the misleading appearance of inflammatory condition as did the MRI. Conclusion – Lymphoma can manifest as LETM. In cases of etiologically unclear atypical LETM in patients older than 40 years, a random skin biopsy (with subcutaneous adipose tissue) from the thigh and from the abdomen is strongly recommended as soon as possible. This may detect IVL and provide the possibility of prompt chemotherapy. In case of suspicion of lymphoma, parallel examination of the CSF by flow cytometry is also recommended. If skin biopsy is negative but lymphoma suspicion remains high, biopsy from other sites (bone marrow, lymph nodes or adrenal gland lesion) or from a simultaneously existing cerebral lesion is suggested, to exclude or prove diffuse large B-cell lymphoma, IVL, or a rare T-cell lymphoma.
Extraskeletal, intradural, non-metastatic Ewing’s sarcoma. Case report
Intracranial localization of Ewing’s sarcoma is considerably very rare. Herein, we present clinical and neuroimaging findings regarding a 4-year-old boy with intracranial Ewing’s sarcoma. He was born prematurely, suffered intraventricular haemorrhage, posthaemorrhagic hydrocephalus developed, and a ventriculoperitoneal shunt was inserted in the newborn period. The patient endured regular follow ups, no signs of shunt malfunction nor increased intracranial pressure were observed. The last neuroimaging examination was performed at 8 months of age. Upon reaching the age of 4 years, repeated vomiting and focal seizures began, and symptoms of increased intracranial pressure were detected. A brain MRI depicted a left frontoparietal space-occupying lesion infiltrating the superior sagittal sinus. The patient underwent a craniotomy resulting in the total excision of the tumour. The histological examination of the tissue revealed a small round blue cell tumour. The diagnosis was confirmed by the detection of EWSR1 gene translocation with FISH (fluorescent in situ hybridization). No additional metastases were detected during the staging examinations. The patient was treated in accordance to the EuroEwing 99 protocol. Today, ten years onward, the patient is tumour and seizure free and has a reasonably high quality of life.
1.
Clinical Neuroscience
[Headache registry in Szeged: Experiences regarding to migraine patients]2.
Clinical Neuroscience
[The new target population of stroke awareness campaign: Kindergarten students ]3.
Clinical Neuroscience
Is there any difference in mortality rates of atrial fibrillation detected before or after ischemic stroke?4.
Clinical Neuroscience
Factors influencing the level of stigma in Parkinson’s disease in western Turkey5.
Clinical Neuroscience
[The effects of demographic and clinical factors on the severity of poststroke aphasia]1.
2.
Clinical Oncology
[Pancreatic cancer: ESMO Clinical Practice Guideline for diagnosis, treatment and follow-up]3.
Clinical Oncology
[Pharmacovigilance landscape – Lessons from the past and opportunities for future]4.
5.